Antimicrobial Finishes: Why Healthcare Facilities are Upgrading Door Hardware in 2026

Healthcare facilities are upgrading their architectural door handles and other door handle hardware with antimicrobial finishes in 2026. This initiative directly addresses evolving infection control standards and the increasing threat of healthcare-associated infections (HAIs). Advancements in material science now offer more effective and durable solutions. This proactive measure significantly reduces pathogen transmission on high-touch surfaces, thereby enhancing patient and staff safety. Studies indicate that antimicrobial finishes on high-touch surfaces substantially reduce pathogen transmission, with one study demonstrating a mean reduction of 1.8 log10 CFU in microbial bioburden. An antimicrobial coating, such as quaternary ammonium-based options, efficiently reduces microbial transmission on environmental surfaces, including every architectural Door Handle and Door Handle, creating safer environments.
Key Takeaways
- Healthcare facilities will upgrade door hardware with antimicrobial finishes in 2026.
- This upgrade helps stop the spread of germs on often-touched surfaces.
- Antimicrobial finishes kill germs all the time, even between cleanings.
- Copper alloys are good because they kill germs throughout the whole material.
- New rules and lessons from the pandemic make these upgrades important.
- These new finishes help lower infection rates and save money.
- They make patients feel safer and protect healthcare workers.
- Facilities must choose the right materials and train staff for this change.
The Escalating Threat: Healthcare-Associated Infections and Surface Contamination

Understanding the Persistent Challenge of HAIs
Prevalence and Impact on Patient Outcomes
Healthcare-associated infections (HAIs) pose a significant and ongoing challenge within medical facilities. These infections develop in patients during their stay or after discharge, often unrelated to their primary diagnosis. Common HAIs include:
- C. diff (Clostridioides difficile) infection: This causes nearly half a million infections annually in the U.S.
- Catheter-associated urinary tract infection (CAUTI): This accounts for 32% of all HAIs, often developing from long-term catheter use.
- Central line-associated bloodstream infection (CLABSI): This makes up 14% of all HAIs, occurring in patients with central lines.
- MRSA (methicillin-resistant Staphylococcus aureus): This common HAI resists certain antibiotics.
- Surgical site infection (SSI): This affects incision wounds, deeper tissues, organs, or surgical implants, accounting for approximately 22% of all HAIs.
- Ventilator-associated pneumonia (VAP): This develops in patients requiring mechanical ventilation, accounting for 15% of all HAIs.
These infections significantly worsen patient outcomes, leading to prolonged hospital stays, increased morbidity, and higher mortality rates. Bacteria like Staphylococcus aureus, Pseudomonas aeruginosa, and E. coli frequently cause HAIs. Other significant pathogens include Methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant Enterococci (VRE), and multidrug-resistant Acinetobacter spp. Fungi such as Candida albicans and viruses like influenza also contribute to the HAI burden.
Economic Burden on Healthcare Systems
HAIs place a substantial economic burden on healthcare systems. They increase treatment costs due to extended hospitalizations, additional medications, and complex interventions. Facilities also incur expenses from managing outbreaks, implementing enhanced infection control measures, and potential legal liabilities. This financial strain diverts resources from other critical areas of patient care and facility improvement.
Door Hardware as a High-Risk Transmission Point
Frequent Touch Points and Pathogen Transfer
Door hardware, including handles, push plates, and pull bars, represents some of the most frequently touched surfaces in any healthcare environment. Patients, staff, and visitors constantly interact with these points. Each touch provides an opportunity for pathogens to transfer from hands to the surface and then to the next person. This constant exchange makes door hardware a critical vector for microbial spread.
Role in Cross-Contamination
Door hardware plays a significant role in cross-contamination within healthcare settings. Pathogens deposited on these surfaces can survive for extended periods, facilitating their transfer between different areas of a facility. Studies have identified various dangerous microorganisms on door hardware surfaces. These include:
- Bacteria: Clostridium difficile, Acinetobacter baumannii, vancomycin-resistant enterococci (VREs), Staphylococcus aureus, Escherichia coli, and Klebsiella pneumoniae.
- Viruses: SARS-CoV-2, Rotavirus, and Norovirus.
The presence of these pathogens on high-touch surfaces underscores the need for continuous infection control strategies beyond routine cleaning.
The Evolution of Infection Control: Beyond Traditional Cleaning
Healthcare facilities recognize the need to move beyond traditional cleaning methods. They seek more robust strategies to combat the persistent threat of healthcare-associated infections (HAIs). This evolution involves integrating advanced technologies with established protocols.
Limitations of Manual Disinfection Alone
Inconsistent Application and Human Error
Manual disinfection, while essential, faces inherent limitations. Human error and inconsistent application often compromise its effectiveness. Staff members, despite training, can miss spots or apply disinfectants incorrectly. This leads to varying levels of cleanliness across different surfaces. Studies consistently show that even with trained personnel, significant areas for improvement exist in terminal disinfection processes.
The following table illustrates the percentage of markings remaining on various high-touch surfaces after manual disinfection, highlighting the inconsistency:
| Surface | Markings Remaining (%) |
|---|---|
| Electrocautery unit | 30.2 |
| Foot pedal | 38.9 |
| Turnover phone | 38.9 |
| Anesthesia cart table | 12.6 |
| Nurses station | 11.8 |
| Supply cabinet doors | 16.6 |
| Mean | 32.9 |
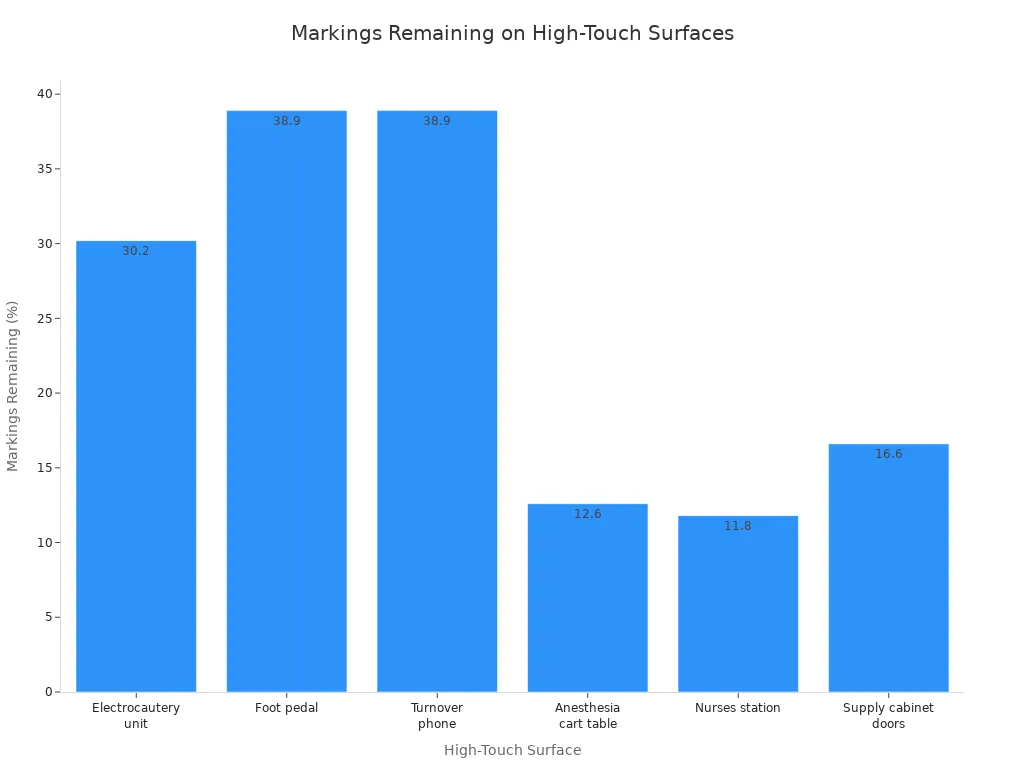
Visual inspection alone proves insufficient for effective terminal disinfection. These inconsistencies underscore the need for enhanced cleaning protocols. Such protocols include staff education or UV light. No-touch room decontamination systems, like UV light, effectively eliminate the "human error" component of the cleaning process. They reduce and eliminate residual pathogens on surfaces.
Challenges with High-Frequency Surfaces
High-frequency surfaces, such as door hardware, present particular challenges for manual disinfection. These surfaces experience constant touching throughout the day. This constant contact means pathogens can quickly recontaminate them after cleaning. Manual cleaning schedules cannot keep pace with the rapid recontamination rate of these critical touchpoints. This creates a continuous cycle of potential pathogen transfer.
The Rise of Passive Infection Control Technologies
Continuous Microbial Inhibition
Passive infection control technologies offer a continuous line of defense against pathogens. Antimicrobial finishes on door hardware provide constant microbial inhibition. These finishes actively work to kill or inhibit the growth of microorganisms on their surfaces. They do this 24/7, without requiring human intervention. This continuous action significantly reduces the bioburden on high-touch surfaces.
Complementary to Active Cleaning Protocols
Passive technologies do not replace active cleaning protocols. Instead, they complement them. They form an additional layer of protection in a comprehensive infection control strategy. Healthcare facilities still perform regular cleaning and disinfection. Antimicrobial finishes enhance these efforts. They ensure a cleaner environment between manual cleaning cycles. This integrated approach creates a more resilient and safer healthcare setting for everyone.
Antimicrobial Finishes: What They Are and How They Work

Healthcare facilities increasingly adopt Antimicrobial Finishes for door hardware. These specialized coatings and materials actively reduce microbial contamination on surfaces. They offer a proactive approach to infection control. Understanding their mechanisms helps facilities choose the most effective solutions.
Defining Antimicrobial Technologies in Door Hardware
Antimicrobial technologies in door hardware involve various active agents. These agents disrupt microbial life cycles. They prevent growth and spread of pathogens.
Silver-Based Antimicrobial Finishes
Silver-based antimicrobial finishes utilize silver ions (Ag+). These ions deactivate bacterial membrane proteins. They bind to thiol groups in these proteins, disrupting their function. Silver-containing coatings show notable antimicrobial performance under specific conditions. High humidity, such as 37°C and over 90% relative humidity, facilitates the ion-exchange reactions. These reactions release silver ions. However, their effectiveness significantly diminishes at typical indoor temperatures and humidity levels. Their performance can become indistinguishable from control surfaces in these conditions.
Copper and Copper Alloy Properties
Copper alloys offer broad-spectrum antimicrobial properties. Copper inactivates pathogens through several mechanisms. It causes leakage of potassium or glutamate from bacterial cells. It also disturbs the osmotic balance within bacteria. Copper binds to proteins that do not require copper for their function. Furthermore, it generates oxidative stress through hydrogen peroxide production. Copper alloys maintain their antimicrobial efficacy across a wider range of conditions. This includes typical indoor environments. Copper and its alloys are antimicrobial throughout their entire structure. Their antimicrobial efficacy persists even if the surface is scratched. This differs from some coatings that can wear away.
Zinc-Based and Other Technologies
Zinc-based technologies also provide antimicrobial benefits. Zinc ions interfere with bacterial metabolism and cell division. Other technologies include quaternary ammonium compounds (Quats) embedded in coatings. These compounds disrupt microbial cell membranes. Photocatalytic nanoparticles, often titanium dioxide, use light to create reactive oxygen species. These species break down organic matter, including microbes.
Durability and Efficacy of Modern Antimicrobial Finishes
Modern antimicrobial finishes offer both durability and high efficacy. They provide long-lasting protection against a wide range of pathogens.
Long-Lasting Performance and Wear Resistance
Modern Antimicrobial Finishes are engineered for extended performance. They withstand the rigors of daily use in healthcare settings. Antimicrobial coatings and embedded treatments generally remain effective for 3–10 years. Specific types of antimicrobial treatments have varying lifespans:
- Silver Ion Infusion: 5–10 years
- Copper Alloy: 10+ years
- Quats Coating: 1–3 years (requires recoating)
- Photocatalytic Nano: 3–5 years
These finishes also boast impressive wear resistance.
| Metric | Antimicrobial Surface | Regular Surface |
|---|---|---|
| Scratch Resistance | High (hardened coatings) | Variable (material-dependent) |
| UV Stability | Excellent (UV-stable additives) | Variable (fades or yellows) |
| Impact Resistance | Good to Excellent | Moderate to Good |
| Chemical Resistance | Broad spectrum | Depends on base material |
Broad-Spectrum Activity Against Pathogens
These finishes exhibit broad-spectrum activity. They effectively target a wide array of bacteria, viruses, and fungi. This includes common HAIs like MRSA, VRE, and C. difficile. The continuous action of these finishes significantly reduces the microbial load on high-touch surfaces. This creates a safer environment for patients and staff.
Why 2026? Key Drivers for Accelerated Adoption of Antimicrobial Finishes
Healthcare facilities are accelerating the adoption of advanced infection control measures. Several critical factors converge in 2026. These factors drive the widespread upgrade to antimicrobial door hardware.
Updated Regulatory Guidelines and Best Practices
Anticipated Changes in Infection Control Standards
The year 2026 marks a pivotal moment for healthcare facilities. Regulatory bodies are introducing significant updates to infection control standards. The Centers for Medicare & Medicaid Services (CMS) released revisions to Appendix A of the State Operations Manual (SOM). These updates include new interpretive guidelines and survey processes. They incorporate guidance from various QSO memos (S&C-16-29, 19-13 (revised), QSO-20-04, 22-20, 23-09, and QSO-23-19) related to infection prevention and control.
Specific areas of focus for compliance in 2026 include:
- Storage of Sterile Instruments: Facilities must ensure proper storage conditions. This includes temperature and humidity control. They must also prevent damage to packaging from stacking or confined spaces.
- Surgical/Procedural Attire: Policies address non-compliance with attire. Examples include long fingernails, artificial nails, loose hair, and exposed jewelry. These measures reduce infection risk.
- Review of Protocols and Standing Orders: Clinical protocols must be up-to-date and evidence-based. Facilities must periodically review and properly document them in patient medical records.
The Joint Commission also introduces new standards for the 'Environment of Care' in 2026. This shifts from rigid checklists to a risk-based management approach. Key changes include:
- Documentation: Facilities move from task logs to code-based risk assessments and system performance data.
- Training: The emphasis is on understanding the 'why' behind practices, not just the 'how'.
- Audits & Rounds: Facilities expect more detailed inspections of fire safety, chemical storage, ventilation, and utility systems.
- EVS & Facilities: Collaboration is required to document and demonstrate safety practices aligned with NFPA standards.
- Leadership: Leaders need to support a culture of compliance. They invest in training, policies, and interdepartmental communication. These comprehensive updates drive facilities to seek advanced solutions like Antimicrobial Finishes.
Industry Recommendations for High-Touch Surfaces
Industry leaders and professional organizations increasingly recommend proactive measures for high-touch surfaces. These recommendations align with the updated regulatory landscape. They emphasize continuous pathogen reduction on surfaces that experience frequent contact. Door hardware falls squarely into this category. Experts advocate for technologies that offer sustained antimicrobial activity. This reduces the reliance on manual cleaning alone. These recommendations push healthcare facilities towards adopting more resilient and self-sanitizing materials.
Post-Pandemic Preparedness and Public Health Focus
Heightened Awareness of Pathogen Transmission
The COVID-19 pandemic profoundly reshaped public and professional understanding of pathogen transmission. Healthcare workers' perceptions of infection prevention and control (IPC) changed significantly. They now place greater value on improved IPC practices. The pandemic created an opportunity to sustain these improved practices. This happened due to increased public knowledge and adaptations in behavior. Examples include improved hand-washing and adoption of non-pharmaceutical interventions.
The World Health Organization (WHO) pandemic declaration significantly increased Google searches related to COVID-19 by more than 20%. This increased public awareness also raised interest in COVID-19 testing. It helped identify new cases early. This collective experience highlighted the critical role of environmental surfaces in disease spread. It underscored the need for robust, continuous infection control measures.
Investment in Resilient Healthcare Infrastructure
This heightened awareness translates into strategic investments in resilient healthcare infrastructure. Facilities now prioritize systems and materials that can withstand future public health crises. They aim to minimize pathogen transmission risks. Upgrading door hardware with advanced materials represents a key part of this investment. It creates environments that are inherently safer and more prepared for emerging threats. This proactive approach protects both patients and staff.
Cost-Benefit Analysis: Long-Term Savings and Patient Outcomes
Reduction in HAI-Related Treatment Costs
Investing in antimicrobial door hardware offers substantial long-term financial benefits. Healthcare-associated infections (HAIs) incur significant treatment costs. These costs include extended hospital stays, additional medications, and complex interventions. The estimated reduction in HAI-related treatment costs for healthcare facilities implementing antimicrobial finishes (specifically ENM coated textiles) is between EUR 304 million and EUR 8038 million annually in the EU. This reduction is noted to be greater than the cost reduction achieved by antiseptics. By reducing HAI rates, facilities can realize considerable savings. This frees up resources for other critical patient care initiatives.
Improved Patient Trust and Satisfaction
Beyond financial savings, the upgrade to antimicrobial door hardware significantly improves patient trust and satisfaction. Patients and their families are increasingly aware of infection risks. They seek facilities that prioritize their safety. A visible commitment to advanced infection control technologies, like antimicrobial surfaces, reassures them. This fosters greater confidence in the healthcare provider. It also enhances the facility's reputation. This leads to improved patient outcomes and overall well-being.
Implementing the Upgrade: Considerations for Healthcare Facilities
Healthcare facilities must carefully plan the upgrade to antimicrobial door hardware. This strategic implementation ensures maximum benefit and seamless integration into existing operations.
Selecting the Right Antimicrobial Hardware
Choosing appropriate antimicrobial hardware requires careful evaluation. Facilities must consider material science, performance, and compliance.
Material Compatibility and Performance Standards
Facilities must select materials that offer lasting antimicrobial efficacy. Some products, like EOScu Solid Surfaces, feature patented synthetic hard surface materials. These materials infuse antimicrobial copper oxide throughout their structure, not just as a coating. Aereus Coated Products also apply a solid copper alloy to items such as bed rails and handles. The antimicrobial effect of these surfaces is permanent. It lasts the entire life of the product. The infused copper does not wear off, wash away, or lose effectiveness. These surfaces are also engineered for durability in healthcare settings. They are compatible with most standard, non-abrasive hospital-grade cleaners and disinfectants. This ensures they maintain their efficacy without compromising cleaning protocols.
Certifications and Regulatory Compliance
Healthcare facilities must ensure all selected antimicrobial hardware meets relevant certifications and regulatory standards. These standards guarantee product safety, efficacy, and environmental responsibility. Compliance with organizations like the Environmental Protection Agency (EPA) for antimicrobial claims is crucial. Facilities should also look for certifications from industry bodies. These certifications confirm the hardware's performance under rigorous testing conditions.
Integration with Existing Infection Control Protocols
Antimicrobial hardware serves as a powerful addition to infection control. It must integrate smoothly with current practices.
Enhancing, Not Replacing, Current Practices
Antimicrobial door hardware enhances existing infection control protocols. It does not replace them. Regular cleaning and disinfection routines remain essential. The antimicrobial surfaces provide a continuous layer of protection between manual cleanings. This dual approach creates a more robust defense against pathogens. Facilities should view this upgrade as an additional tool in their comprehensive infection prevention strategy.
Staff Training and Awareness
Effective implementation requires thorough staff training and awareness. All personnel, including environmental services, nurses, and maintenance staff, must understand the new hardware. They need to know its benefits and proper maintenance. The Copper Development Association (CDA) launched two videos for this purpose. These videos educate hospital executives and staff on the benefits and ease of installing and maintaining antimicrobial copper surfaces. Their titles are "Installing Antimicrobial Copper Components" and "Cleaning and Maintaining Antimicrobial Copper Surfaces." This training ensures staff correctly handle and maintain the hardware. It also reinforces the facility's commitment to patient and staff safety.
The Impact of Antimicrobial Finishes on Patient and Staff Safety
The strategic upgrade to door hardware with antimicrobial properties brings profound benefits. It directly enhances the safety and well-being of everyone within healthcare environments. These advanced materials create a continuous line of defense against pathogens. They significantly reduce the risks associated with high-touch surfaces.
Reducing Pathogen Transmission on High-Touch Surfaces
Antimicrobial door hardware plays a crucial role in breaking the chain of infection. It actively works to keep surfaces cleaner.
Decreased Risk of Cross-Contamination
Antimicrobial properties in frequently touched surfaces like Door Handles help healthcare facilities maintain higher hygiene standards. This reduces the likelihood of cross-contamination between healthcare workers, patients, and environmental surfaces. It enhances overall infection control and creates safer environments. These coatings, enriched with antimicrobial agents, impede microbial proliferation. This decreases the risk of infection transmission in healthcare settings. This applies to various surfaces, including medical devices, hospital furniture, and textiles. Even textile materials in healthcare environments, such as uniforms and bed linen, are prone to microbial contamination.Impregnating these textiles with antimicrobial substances minimizes contamination and microbial load. This reduces biological risks and cross-contamination.
Enhanced Environmental Hygiene
Optimal environmental hygiene practices are integral to patient safety. They are a key component for improving infection prevention and control. A systematic review demonstrates a strong relationship between interventions to improve environmental hygiene (HEH) and a reduction in both environmental bioburden and in patient colonization or healthcare-associated infections (HAIs). Healthcare institutions can lower their HAI rates by improving HEH practices.
Various studies highlight the impact of environmental hygiene interventions on patient outcomes:
| Study Title | Study Design | Key Intervention | Patient Outcome | Grade |
|---|---|---|---|---|
| Prospective cluster controlled crossover trial to compare the impact of an improved hydrogen peroxide disinfectant and a quaternary ammonium-based disinfectant on surface contamination and health care outcomes | Randomized Controlled Trial | Daily cleaning with liquid hydrogen peroxide, staff feedback | No significant reduction of composite colonization and infection outcome (HAI and acquisition for VRE and MRSA, HAI for C. difficile) | A |
| Environmental disinfection with photocatalyst as an adjunctive measure to control transmission of methicillin-resistant Staphylococcus aureus: a prospective cohort study in a high-incidence setting | Before and After Prospective | Photocatalyst antimicrobial coating (TiO2) | Significant reduction in MRSA acquisition rate; no significant reduction in MRSA and C. difficile incidence rate; significant reduction in hospital-acquired pneumonia incidence rate | B |
| Clostridium difficile infection incidence: impact of audit and feedback programme to improve room cleaning | Retrospective Before and After Study | Online training, monitoring, weekly feedback | Reduction of hospital-acquired C. difficile infection incidence following intervention; accelerated rate of decline | C |
| A Multicenter Randomized Trial to Determine the Effect of an Environmental Disinfection Intervention on the Incidence of Healthcare-Associated Clostridium difficile Infection | Randomized Controlled Trial | Training and monitoring of EVS personnel with feedback | No reduction in the incidence of healthcare-associated C. difficile infection | B |
| Environmental services impact on healthcare-associated Clostridium difficile reduction | Retrospective Quasi-Experimental Design | Culture of safety with constructive feedback, education, auditing certifications, and accountability | Significant reduction in healthcare-associated Clostridium difficile infections | B |
| Comparison of the effect of detergent versus hypochlorite cleaning on environmental contamination and incidence of Clostridium difficile infection | Prospective Quasi-Experimental Study | Hypochlorite with training | Significant reduction in C. difficile infection associated with hypochlorite use in one ward | B |
| Control of endemic multidrug-resistant Gram-negative bacteria after removal of sinks and implementing a new water-safe policy in an intensive care unit | Prospective Before and After Study | Deep cleaning and disinfection of drains and valves; antibacterial water filters; external cleaning with microfiber cloths and hypochlorite solution | Significant reduction of MDR-Gram-negative bacteria incidence rates | C |
| Reducing health care-associated infections by implementing separated environmental cleaning management measures by using disposable wipes of four colors | Prospective Before and After Study | Training, education, and awareness regarding cleaning and 4 color-coded reusable wipes | No reduction in HAI density after intervention, but during follow-up period | C |
| An environmental cleaning bundle and health-care-associated infections in hospitals (REACH): a multicentre, randomised trial | Randomized Controlled Trial | Training, auditing, feedback, enhanced cleaning practices, disposable wipes | Significant reduction of VRE infections; no significant changes in S. aureus bacteremia and C. difficile infections | A |
| Implementation of human factors engineering approach to improve environmental cleaning and disinfection in a medical center | Prospective Before and After Study | Education, feedback, redesigned workflow, bleach dilution method, checklist-form reminder | Significant reduction in total MDRO colonization, but no reduction in HAI | D |
This table illustrates that various interventions, including advanced cleaning methods and materials, contribute to better environmental hygiene. Antimicrobial door hardware adds a continuous layer of protection. It supports these efforts by constantly reducing microbial load on high-touch surfaces.
Creating Safer Healthcare Environments
The adoption of antimicrobial door hardware contributes to a holistic improvement in the healthcare environment.
Improved Patient Outcomes and Well-being
A cleaner, safer environment directly translates to improved patient outcomes. Reduced rates of HAIs mean fewer complications, shorter hospital stays, and faster recovery times for patients. Patients experience less anxiety about infection risks. This contributes to their overall well-being and satisfaction with their care. Facilities demonstrate a clear commitment to patient safety. This fosters greater trust and confidence in the healthcare system.
Increased Staff Confidence and Protection
Antimicrobial finishes contribute to increased staff confidence and protection against infection. They continuously suppress microbial growth. This reduces contamination levels between cleanings. This leads to improved hygiene confidence among staff and patients. It also results in better workflow efficiency and reduced cross-contamination risks. These materials provide continuous protection between cleaning cycles, especially in high-touch areas. They meet strict safety standards for human contact. This ensures their safety for use across all hospital departments. Staff members feel more secure in their work environment. This allows them to focus more effectively on patient care.
The 2026 upgrade to antimicrobial door hardware represents a critical advancement in proactive infection control. This strategic investment significantly impacts patient safety, operational efficiency, and the overall healthcare environment. It underscores the importance of continuous innovation in infection prevention for a healthier and more secure future. Facilities prioritize patient well-being. They also enhance operational effectiveness. This forward-thinking approach sets new standards for healthcare safety.
FAQ
What are antimicrobial finishes on door hardware?
Antimicrobial finishes are specialized coatings or materials. They actively kill or inhibit the growth of microorganisms on their surfaces. These finishes help reduce pathogen transmission on high-touch areas like door handles.
Why are healthcare facilities upgrading door hardware in 2026?
Healthcare facilities are upgrading due to new regulatory guidelines and best practices. The post-pandemic focus on public health also drives this change. Facilities aim to enhance patient and staff safety by reducing healthcare-associated infections (HAIs).
Do antimicrobial finishes replace traditional cleaning methods?
No, antimicrobial finishes do not replace traditional cleaning. They complement existing infection control protocols. These finishes provide continuous protection between manual cleaning cycles. This creates a more robust defense against pathogens.
What types of antimicrobial materials are used in door hardware?
Common antimicrobial materials include silver-based finishes, copper alloys, and zinc-based technologies. Copper alloys offer broad-spectrum efficacy throughout their entire structure. Other options include quaternary ammonium compounds and photocatalytic nanoparticles.
How long do modern antimicrobial finishes remain effective?
The lifespan of antimicrobial finishes varies by type. Silver ion infusion can last 5–10 years. Copper alloys offer 10+ years of efficacy. Quats coatings typically last 1–3 years. Photocatalytic nano finishes last 3–5 years.
How do antimicrobial finishes benefit patients?
Antimicrobial finishes reduce the risk of healthcare-associated infections. This leads to fewer complications and shorter hospital stays. Patients experience less anxiety about infection. This improves their overall well-being and satisfaction with care.
How do these upgrades protect healthcare staff?
Antimicrobial finishes continuously suppress microbial growth on high-touch surfaces. This reduces staff exposure to pathogens. Staff members feel more secure in their work environment. This allows them to focus more effectively on patient care.
What should facilities consider when selecting antimicrobial hardware?
Facilities should consider material compatibility and performance standards. They must also check for certifications and regulatory compliance. Integration with existing infection control protocols and staff training are also crucial for successful implementation.










